What is Pelvic organ prolapse?
WOMENS WELLNESS
Pelvic organ prolapse can occur when the muscles or tissues that usually support the pelvic organs become weak or loose. When these muscles and tissues are weak, the organs can drop or bulge from their normal position.
How do I know if I have pelvic organ prolapse?
The symptoms of pelvic organ prolapse include;
- Lumps or bulges in the vagina
- Discomfort inside the vagina
- The sensation that you are sitting on a small ball
- Urinary incontinence
- Heaviness around the lower tummy and genitals
- Discomfort or numbness during sex
What causes pelvic organ prolapse?
Pelvic organ prolapse is caused when the muscles and tissues that normally support the pelvic organs are weakened. The cause of this includes;
- Past hysterectomy
- Being overweight
- Ageing and Menopause
- Pregnancy and childbirth
- Heavy lifting
- Certain Health conditions
How to treat pelvic organ prolapse?
The type of treatment required for pelvic organ prolapse will depend on the severity of your symptoms.
Emsella
We believe one of the most effective treatments for pelvic organ prolapse is Emsella treatment.
Emsella pelvic floor therapy is a non-surgical FDA approved treatment that is very effective at strengthening the pelvic floor and relieving the symptoms of pelvic organ prolapse.
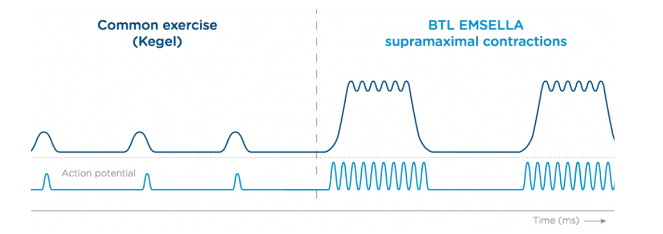
Emsella works by applying High-Intensity Focused Electromagnetic technology (HIFEM) to stimulate the pelvic floor muscles and restore neuromuscular control. A single Emsella session can bring thousands of supramaximal pelvic floor muscle contractions which are very important in the muscle re-education on incontinent patients. It is reported that one session of Emsella is the equivalent of 11000 Kegel exercises.
The benefits of Emsella treatment
- FDA Cleared to improve urinary incontinence & vaginal laxity
- Patients remain fully clothed throughout treatment
- 75% reduction in pad usage
- Non-invasive & Non-surgical
- Walk-in, walk out procedure
- No recovery or downtime
- 95% of BTL Emsella patients experienced noticeable improvement
- Treats entire pelvic floor area in 30 minutes
Other pelvic organ prolapse treatment methods are;
Lifestyle Changes
There are various lifestyle changes that may be suggested which can help to ease the symptoms of pelvic organ prolapse and stop the prolapse from getting worse. These include;
- Avoid lifting heavy objects
- Eat a high fibre diet
- Stop smoking
- Avoid high impact exercises
Pelvic Floor Exercises
Pelvic floor exercises or Kegel exercises are a series of movements that can help to strengthen the muscles that usually support the pelvic organs. As pelvic organ prolapse is caused by a weak pelvic floor, strengthening this area can really help to treat pelvic organ prolapse. You can feel your pelvic floor when you try to stop the flow of urine when going to the toilet. One of the most common exercises to strengthen the pelvic floor is very simple;
- Sit comfortably
- Identify the correct muscles
- Squeeze the muscles for 5 seconds
- Release the muscles for 5 seconds
- Hold each squeeze for a few seconds
- Repeat this 10 times, 3 times a day
- Gradually build up the number of squeezes over time
Physiotherapy for the pelvic floor
You may be referred to a pelvic floor physiotherapist to help you manage incontinence, pelvic organ prolapse and pelvic pain. Physiotherapy treatment usually involves; pelvic floor training exercises as mentioned above, manual therapy or safe rehabilitation following pelvic floor surgery.
What does a pelvic floor physiotherapist do?
Seeing a pelvic floor physiotherapists can help you to rehabilitate the pelvic floor muscles through exercises, biofeedback (electronic monitoring), and the manual treatment of the muscle. They will also be able to offer advice on good bladder and bowel habits, sexual difficulties, pelvic pain, daily activities and fitness.
It can take 3-5 months to start noticing results from pelvic floor exercises and you will need to keep practicing the exercises at least once a day in order to maintain the improvements.
Vaginal Pessaries
Vaginal pessaries are devices that are inserted into the vagina where they stay to support the vaginal walls and pelvic organs. Usually made from latex or silicone, the devices come in different sizes to help reduce the symptoms of moderate to severe prolapses. Vaginal pessaries will need to be replaced regularly and, in some cases, can cause stress incontinence and other infections.
Surgery
There are 4 types of surgery options for pelvic organ prolapse;
- Surgical Repair
- Vaginal Mesh Surgery
- Hysterectomy
- Closing the vagina
Surgery for pelvic organ prolapse often involves lifting and supporting the pelvic organs by stitching them into place or supporting the existing tissues to make them stronger. Surgery is always carried out under general anaesthetic and the technique used will depend on the severity of the prolapse. Pelvic organ prolapse surgery does often come with a hospital stay and substantial downtime with the general recommendation being 6-12 weeks off work to recover.
The NHS no longer offers vaginal mesh surgery which is where a piece of synthetic mesh is inserted into the body to hold the pelvic organs in place.
Why choose The Private Clinic?
The Private Clinic are a multi-award-winning Cosmetic Surgery provider with over 40 years’ experience in Medical Cosmetic procedures and advanced non surgical non invasive treatments. We are proud to have pioneered the widest range of minimally-invasive, surgical, medical-cosmetic and aesthetic treatments catered to the individual needs of our patients
To find out more about pelvic organ prolapse treatment with Emsella, give us a call on 0333 920 2471 or book a free consultation at our clinic in Leeds using our online contact form.




