
Phlebectomy Varicose Vein Treatment
A Phlebectomy is a minimally invasive varicose vein treatment. It uses a small scalpel and hook to remove superficial or ‘surface’ varicose veins that lie just beneath the skin’s surface. This age-old tried-and-tested technique is one of the lesser-used methods to remove varicose veins today. However, there are certain situations where the technique still proves beneficial.
What is a Phlebectomy?
A phlebectomy is simply a form of varicose vein “keyhole” or microsurgery. It physically removes surface varicose veins with a specialised phlebectomy hook device. Tiny micro incisions of around 2mm are made at the site of the varicose vein before a phlebectomy hook is inserted to pull it out. No stitches are required and the incision heals rapidly due to the nature of the tiny micro punctures. This makes the procedure much less risky and complicated than traditional ‘vein stripping,’ which is outdated and was associated with a poor success rate and long recovery times.

What does Phlebectomy mean?
The medical term ‘Phlebectomy’ is comprised of two medical phrases. The word ‘phleb’ means ‘vein’ while the term ‘ectomy’ means ‘to remove or take out.’
It is also known as a micro, or ‘mini’ phlebectomy thanks to its minimally invasive design. Some clinics also call it an ‘avulsion’ therapy.
What is an Ambulatory Phlebectomy?
Modern-day phlebectomies are sometimes known as ambulatory phlebectomies. This term describes how phlebectomies are now carried out as simple walk-in, walk-out procedures under local anaesthetic. This is in a similar way to other minimally invasive treatments like EVLA. Patients can have their veins treated as an outpatient with no need for an overnight hospital stay.
What veins can be treated with a Phlebectomy?
An ambulatory phlebectomy is used to treat bulging veins that appear on the surface of the skin. It is also usually recommended if other vein treatments have not worked to reduce the appearance of the surface bulges. For example, when the size and pressure of blood in a vein is too great for a sclerotherapy treatment, and the skin characteristics of the patient make it difficult for sclerotherapy to achieve desired cosmetic outcomes, phlebectomy is used as an alternative.

Phlebectomy with EVLA
It is also often used in combination with EVLA, which fixes the deeper ‘venous reflux’ cause of varicose veins. While EVLS corrects venous reflux issues, it sometimes fails to minimise the bulging appearance of shallow veins. In such circumstances, phlebectomy is recommended as an effective procedure to physically remove the shallow twisted and bulging veins. These are known as “varices,” and phlebectomies are highly successful at removing these unsightly veins. However, the treatment does not fix the underlying cause of varicose veins. This is why it is usually combined with a treatment like EVLA which works to specifically fix the incorrect ‘venous reflux’ blood flow – where blood flows backwards inside the vein due to faulty vein valves, leading to swollen and enlarged varicose veins.
Why use Phlebectomy to treat varicose veins?
The main advantage of having a phlebectomy procedure is the instant visible removal of bulging surface veins, which can often affect patient self-confidence. For cosmetic reasons, this makes the procedure a great choice for patients who want to reduce the visible signs of their surface veins in a rapid way. It offers a quick remedial solution to fix enlarged surface veins if a person has a big upcoming event to prepare for, like a wedding or holiday for example like a wedding to prepare for. However, your consultant vascular surgeon will always advise on whether this option is the best treatment for you after assessing your veins during a detailed consultation.
Benefits of Phlebectomy
A phlebectomy is a highly successful procedure when performed on the ideal candidate. With a proven long-term success rate of 90%, it has great effectiveness at noticeably reducing the appearance of shallow surface varicose veins. See below for the key benefits:
- Minimally invasive treatment
- Walk-in, walk-out procedure
- Only requires local anaesthetic
- Impressive success rate when used in combination with other procedures like Endovenous Laser Ablation (EVLA) and foam sclerotherapy
- Fast recovery times, with an almost immediate return to normal daily activities
- Leaves no marks or obvious scarring
- About 95% of phlebectomy patients experience significant relief from pain and symptoms
The Phlebectomy Consultation
The first part of a varicose vein treatment involves a consultation with one of our professional consultant vascular surgeons. The vascular surgeon will assess your surface veins to see if they are suitable for the phlebectomy procedure. In most cases, phlebectomy will be offered in partnership with other complementary treatments like EVLA if required. The consultant will explain the procedure to you to make it clear, along with the expected results of the treatment.
This treatment is relatively simple to perform so does not usually require a duplex ultrasound scan to determine the exact location and structure of the vein. Superficial veins are clearly visible as bulges through the skin, unlike deeper truncal veins treated with methods like EVLA. This makes the veins easy to treat without the need for a scan in most cases.
The Phlebectomy Procedure
An ambulatory phlebectomy treatment is carried out as a day-case microsurgery operation using local anaesthetic and is usually completed between 30 minutes to one hour.
Before a patient is treated, the vascular surgeon will mark up the position of the patient’s bulging veins by drawing around them with a marker. This needs to be done while the patient is standing, as the varicose veins will deflate and disappear from view as soon as the patient lays down on the operating table.
The skin across the treatment area is cleaned before the patient is put into a surgical gown to prepare for the micro-incision. A local anaesthetic is then injected under the skin to make the veins and surrounding skin numb. A small scalpel is then used to make a tiny micro-puncture to allow the vascular surgeon to physically remove the damaged varicose vein. A very fine 2mm blade is used for this incision, and while it may feel slightly uncomfortable, the patient won’t feel any pain due to the strength of the local anaesthetic.
A very fine phlebectomy hook is then attached to the vein to pull it up and remove it from the body. Enlarged varicose veins are easily collapsible, so the procedure is relatively straightforward to complete. The incisions made during the procedure are so small that stitches are not required, and the wound will heal quickly by itself. A surgical dressing will be applied at the incision point to facilitate this natural process.
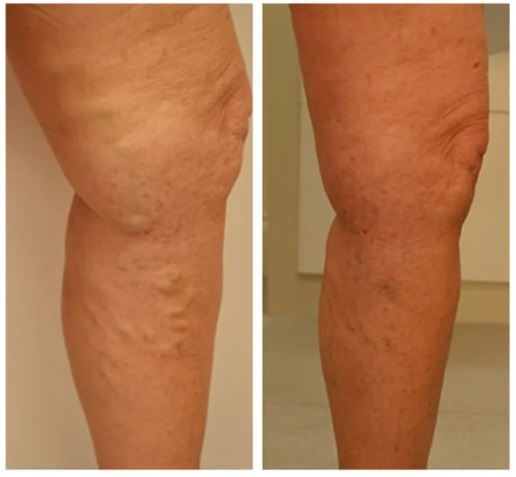
What is the success rate of Phlebectomy?
A phlebectomy has a 90% long-term success rate when performed for appropriate medical reasons on an ideal candidate. Most patients fully recover from the procedure around 6 weeks after the treatment. The phlebectomy before and after photo below showcases this success for one of our patients:
Phlebectomy Aftercare
In-Clinic Aftercare
Immediately after the procedure, your vascular surgeon will apply surgical tape and a dressing to close the tiny micro-incision. This should be left on for 3 days to allow the incision to heal. Your leg will also be wrapped in a compression bandage to secure the treatment area and aid recovery.
At-Home Aftercare
Patients should avoid driving for 24 hours after having a phlebectomy due to the after-effects and numbness of the local anaesthetic. Compression stockings and bandages should be worn for 2-3 weeks after the procedure. Patients can perform almost all of their usual activities the day after having their treatment when the stockings are being worn. You can expect to resume day-to-day activities within 24 hours, although strenuous activities like going to the gym should be avoided for approximately 2 weeks.
What are the side effects of Phlebectomy?
Most ambulatory phlebectomy procedures go according to plan thanks to the procedure’s extremely high success rate. However, as the procedure is microsurgery, there is potential for some patients to experience side effects. The most common is bruising around the treatment area. This usually disperses around 1-3 weeks post-treatment. Some patients may also experience pain or aching at the treatment area. But this can be rectified by taking over-the-counter analgesic medications for targeted pain relief.

What is the difference between Phlebectomy and Vein Stripping?
Vein stripping is the old method of surgically removing varicose veins. However, this stripping process often led to considerable pain and bruising for the patient. It also had a relatively high failure rate, with only 50% of cases being successful. Today, leading vein clinics offer up more minimally invasive methods like EVLA and phlebectomies. While phlebectomy is still a surgical method, the incisions are tiny. The healing is fast, and the physical removal of the shallow vein is not as destructive as deep vein stripping.
Phlebectomy at The Private Clinic
At The Private Clinic, we have been performing varicose vein treatments for over 40 years. We work with the most highly trained surgeons who have been instrumental in developing today’s leading treatments in the UK, including EVLA. We perform over 7,000 vein treatments each year, and our patients commend us for our high standards of care and exceptional results, which can be seen in our 5-Star Trustpilot score.
To find out more about our Phlebectomy treatments, or any of our other varicose vein procedures, fill out our varicose vein online contact form. Alternatively, you can call us directly on 0333 920 2471. We have easily accessible clinic locations throughout the country in London Harley Street, Birmingham, Northampton and Bournemouth.




