Get Body Confident
VEINS
Tesco Living
Concern: Can I do anything to reduce my varicose veins?
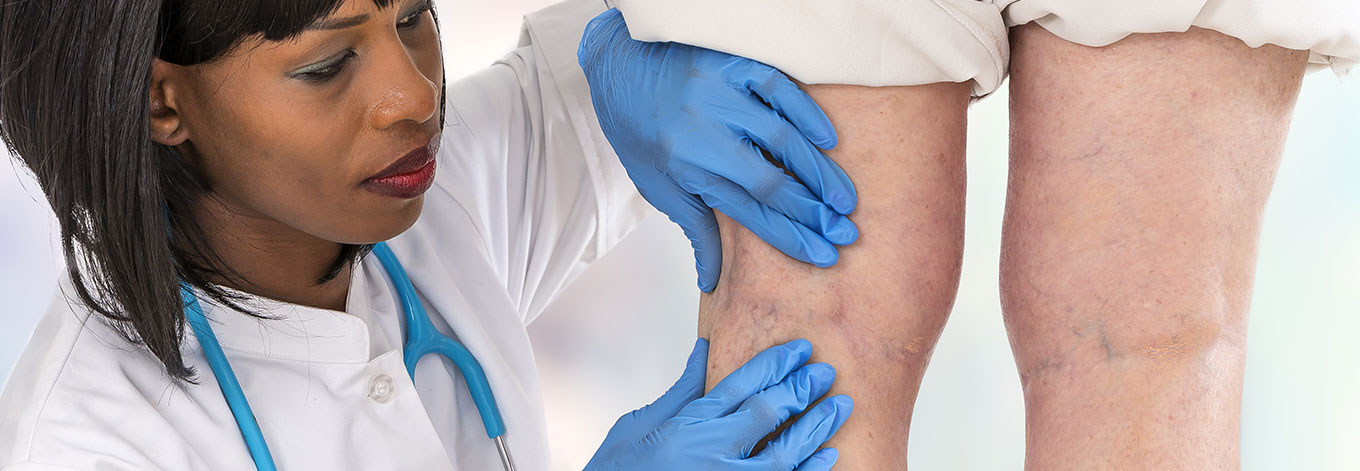
Swollen, blue/black leg veins are a sure-fire way to make you cover up. But if varicose veins are making you miserable – and your legs unsightly – there are effective medical treatments available. Varicose veins develop when the small valves inside the veins stop working properly. If these valves get damaged or weaken, the blood gets trapped inside the vein and over time it becomes swollen and enlarged.
“Around three in 10 adults will, at some point in their life, develop varicose veins,” says Mr Constantinos Kyriakides, a Consultant Vascular Surgeon at The Private Clinic, Harley Street. “Although varicose veins are often treated for cosmetic purposes, they can also have greater health implications than most of us are aware of.” Aching, itching, and a feeling of heaviness in the legs are all common complaints. As with any invasive surgery, it’s always important to undergo a thorough examination before you decide on any procedures.
Solution
If you are suffering pain or discomfort from your varicose veins, it’s best to visit your GP for advice. However, unless the veins are causing you serious health concerns, it’s unlikely you’ll get treatment for them on the NHS. If you want veins removed for cosmetic reasons and are prepared to go privately, sclerotherapy is a tried-and-tested treatment for smaller veins. This involves injecting a chemical into the vein to close it completely, so that it no longer carries blood. Although it can improve the appearance of your legs, they may still ache. And after the injection, you’ll have to wear support stockings for three to six weeks.
For more serious veins, the best treatment is called Endovenous Laser Ablation (EVLA) – a walk-in, walk-out procedure, performed under local anesthetic. Although it’s expensive (prices start at around £2,150) it’s minimally invasive and is an arguably more effective alternative to the more invasive vein stripping method, which although cheaper, is a major surgical procedure that usually requires general anesthetic and up to six weeks ‘down time’.
“The results of EVLA have been shown to last longer than those which can be achieved through vein stripping, while research has shown that veins which have been stripped grow back in almost a quarter of cases,” comments Mr Kyriakides. With an EVLA treatment, first an ultrasound scan is used to mark the position of the veins. Local anesthetic is injected around the vein to ease any discomfort and then a fine probe is then inserted through a very small incision, usually close to the patient’s knee. Next, laser energy is delivered in short or continuous pulses to seal the faulty vein so that blood can no longer flow through it. The procedure usually takes less than 30 minutes and you can go home afterwards.